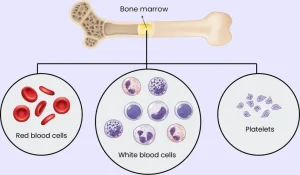
Overview
Myelofibrosis is a rare, chronic bone marrow disorder in which scar tissue gradually replaces healthy bone marrow. This scarring disrupts the body’s ability to produce normal blood cells, leading to anemia, weakness, and enlargement of organs such as the spleen and liver. Myelofibrosis is classified as a type of myeloproliferative neoplasm and may occur on its own or develop from other bone marrow diseases.
The condition usually progresses slowly, but in some cases it can become more aggressive or transform into acute leukemia. Management focuses on symptom relief, slowing disease progression, and improving quality of life.
Symptoms
Symptoms of myelofibrosis often develop gradually and may vary in severity.
Common symptoms include:
-
Fatigue and weakness
-
Shortness of breath
-
Pale skin due to anemia
-
Easy bruising or bleeding
-
Frequent infections
-
Bone or joint pain
-
Night sweats
-
Fever
-
Unintentional weight loss
-
Abdominal discomfort or fullness from an enlarged spleen
Some individuals may be asymptomatic in the early stages and diagnosed through routine blood tests.
Causes
Myelofibrosis is caused by genetic mutations in blood-forming stem cells within the bone marrow. These mutations lead to abnormal blood cell production and stimulate excess fibrous tissue formation in the marrow.
Known contributing factors include:
-
Acquired genetic mutations such as JAK2, CALR, or MPL
-
Abnormal signaling that causes overproduction of certain blood cells
-
Progression from other myeloproliferative disorders, such as polycythemia vera or essential thrombocythemia
The exact reason these mutations occur is often unknown.
Risk Factors
Several factors may increase the likelihood of developing myelofibrosis.
Risk factors include:
-
Older age, typically over 50 years
-
History of other bone marrow disorders
-
Presence of specific genetic mutations
-
Long-term exposure to certain chemicals or radiation
-
Family history of blood disorders, in rare cases
Both men and women can be affected, though the condition is more common in older adults.
Complications
Myelofibrosis can lead to a number of serious complications as the disease progresses.
Potential complications include:
-
Severe anemia requiring blood transfusions
-
Increased risk of infections
-
Excessive bleeding due to low platelet levels
-
Enlarged spleen causing pain or digestive problems
-
Portal hypertension
-
Acute myeloid leukemia transformation
-
Reduced physical functioning and quality of life
Regular monitoring helps detect and manage complications early.
Prevention
There is no proven way to prevent myelofibrosis, as it often develops due to spontaneous genetic mutations. However, certain steps may support overall health and early detection.
Preventive and supportive measures include:
-
Avoiding exposure to harmful chemicals and radiation when possible
-
Maintaining regular medical checkups
-
Monitoring blood counts if there is a history of bone marrow disorders
-
Prompt evaluation of unexplained fatigue, anemia, or abdominal fullness
-
Following medical advice for long-term disease management
Early diagnosis and individualized treatment plans can help control symptoms, reduce complications, and improve long-term outcomes for individuals with myelofibrosis.
Advertisement