Overview
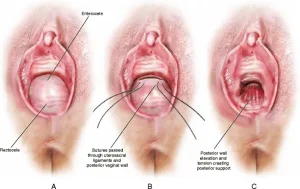
Posterior Vaginal Prolapse, also known as a rectocele, occurs when the wall between the vagina and the rectum weakens, allowing the rectum to bulge into the vaginal space. This condition is often associated with childbirth, aging, or chronic pressure on the pelvic floor. A rectocele can range from mild to severe and may cause discomfort, difficulties with bowel movements, and reduced quality of life.
Symptoms
Common symptoms of a posterior vaginal prolapse (rectocele) include:
-
A feeling of bulging or pressure in the vagina
-
Difficulty with bowel movements or a sensation of incomplete evacuation
-
Straining during defecation
-
Discomfort or pain in the pelvic region
-
Vaginal or rectal fullness, especially when standing or straining
-
Symptoms may worsen with activity and improve when lying down
Causes
Rectocele develops due to weakening of the supportive tissues of the pelvic floor:
-
Vaginal childbirth causing stretching or injury to pelvic muscles and connective tissue
-
Aging and natural decline in tissue elasticity
-
Chronic constipation or straining during bowel movements
-
Previous pelvic surgery or hysterectomy
-
Obesity or repetitive heavy lifting that increases pelvic pressure
Risk factors
Factors that increase the risk of developing a rectocele include:
-
Multiple vaginal deliveries, especially with large babies
-
Advancing age and menopause, which reduce estrogen and tissue strength
-
Chronic constipation or straining
-
Obesity and increased intra-abdominal pressure
-
Genetic predisposition to weak connective tissues
Complications
If untreated, posterior vaginal prolapse can lead to:
-
Persistent pelvic discomfort or pain
-
Difficulty with bowel movements, including fecal incontinence in severe cases
-
Sexual discomfort or pain during intercourse
-
Increased risk of urinary or vaginal infections due to impaired pelvic support
-
Reduced quality of life and social limitations
Prevention
Preventive measures and management strategies include:
-
Practicing pelvic floor exercises (Kegels) to strengthen supporting muscles
-
Avoiding chronic straining during bowel movements by maintaining a high-fiber diet and proper hydration
-
Maintaining a healthy weight to reduce pelvic pressure
-
Using proper techniques for lifting heavy objects
-
Seeking early medical evaluation for pelvic discomfort or bulging to prevent worsening
Early recognition and pelvic floor rehabilitation can help manage posterior vaginal prolapse, reduce symptoms, and improve overall pelvic health.
Advertisement