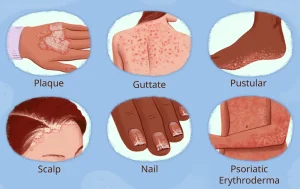
Overview
Psoriasis is a chronic autoimmune skin condition that causes skin cells to multiply faster than normal. This rapid growth leads to the buildup of thick, scaly patches on the skin. These patches are often red, inflamed, and covered with silvery-white scales. Psoriasis commonly affects areas such as the scalp, elbows, knees, and lower back, but it can appear anywhere on the body.
The condition tends to occur in cycles, with periods of flare-ups followed by periods of improvement. Psoriasis is not contagious and cannot be spread from person to person. Although it is a long-term condition, proper treatment and lifestyle management can help control symptoms and reduce flare-ups.
Symptoms
Symptoms of psoriasis vary depending on the type and severity of the condition.
Common symptoms include:
-
Red patches of skin covered with thick, silvery scales
-
Dry, cracked skin that may bleed
-
Itching, burning, or soreness
-
Thickened or ridged nails
-
Small scaling spots, often seen in children
-
Swollen or stiff joints in some cases
Symptoms may range from mild irritation to severe skin involvement that affects large areas of the body.
Causes
Psoriasis occurs due to an abnormal immune system response that speeds up the life cycle of skin cells. Normally, skin cells grow and shed over several weeks, but in psoriasis this process happens within a few days.
This rapid turnover causes skin cells to accumulate on the surface of the skin, forming thick, scaly patches. The exact reason for this immune system malfunction is not fully understood, but it likely involves both genetic and environmental factors.
Certain triggers may worsen or activate psoriasis, including infections, stress, skin injuries, cold weather, and some medications.
Risk Factors
Several factors can increase the likelihood of developing psoriasis.
These include:
-
Family history of psoriasis
-
Immune system disorders
-
Severe stress
-
Obesity
-
Smoking
-
Certain infections such as strep throat
-
Skin injuries such as cuts, burns, or insect bites
People with psoriasis may also have a higher risk of developing psoriatic arthritis.
Complications
Psoriasis can lead to several complications, especially if the condition is severe or poorly controlled.
Possible complications include:
-
Psoriatic arthritis
-
Increased risk of heart disease
-
Type 2 diabetes
-
High blood pressure
-
Depression and anxiety
-
Eye inflammation
-
Metabolic syndrome
Managing psoriasis effectively can help reduce the risk of these associated health problems.
Prevention
There is no known way to completely prevent psoriasis because it is largely influenced by genetic and immune system factors. However, certain steps may help reduce flare-ups and manage symptoms.
Helpful preventive measures include:
-
Keeping the skin moisturized
-
Managing stress effectively
-
Avoiding smoking and excessive alcohol consumption
-
Maintaining a healthy weight
-
Protecting the skin from injuries
-
Identifying and avoiding personal triggers
Following a consistent treatment plan and regular medical care can help keep psoriasis symptoms under control and improve overall quality of life.
Advertisement