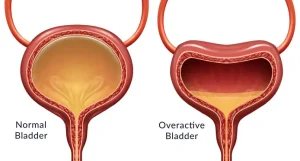
Overview
Diagnosis
To diagnose an overactive bladder, your healthcare professional will start by checking for infections or blood in your urine and evaluating how well your bladder empties. A full assessment may include:
-
Medical history to understand your symptoms and overall health.
-
Neurological exam to identify any sensory or reflex issues.
-
Physical exam, including a rectal exam or a pelvic exam in women.
-
Urine sample to check for infection, blood, or other abnormalities.
Tests of bladder function (urodynamic tests)
These tests assess how well your bladder stores and empties urine. They are often performed by a specialist, though they may not always be required for diagnosis.
Common urodynamic tests include:
-
Measuring urine left in the bladder after urination (postvoid residual). This may be done with an ultrasound or a catheter to determine if your bladder empties completely.
-
Measuring urine flow rate using a device called a uroflowmeter, which records how much and how fast you urinate.
-
Testing bladder pressures (cystometry), where your bladder is filled slowly with warm fluid through a catheter to measure the pressure and assess how full your bladder is when you first feel the urge to urinate.
Once your healthcare provider reviews your results, a personalized treatment plan is developed.
Treatment
A combination of approaches is often most effective for managing overactive bladder symptoms.
Behavioral therapies
Behavioral therapies are the first line of treatment and are highly effective without causing side effects. These may include:
-
Biofeedback to help you recognize and control bladder muscle contractions.
-
Bladder training to gradually increase the time between trips to the bathroom using a bladder diary.
-
Maintaining a healthy weight to reduce pressure on the bladder.
-
Intermittent catheterization to help empty the bladder completely when necessary.
-
Pelvic floor muscle exercises (Kegel exercises) to strengthen the pelvic muscles and urinary sphincter.
Kegel exercises should be performed regularly for at least six weeks for best results.
Medications
Your healthcare provider may recommend medicines to help relax the bladder muscles and reduce urge incontinence. Common options include:
-
Fesoterodine (Toviaz)
-
Mirabegron (Myrbetriq)
-
Oxybutynin (Ditropan XL, Oxytrol, Gelnique)
-
Solifenacin (Vesicare)
-
Tolterodine (Detrol)
-
Trospium
-
Vibegron (Gemtesa)
Vaginal estrogen therapy after menopause may also help strengthen pelvic tissues.
Possible side effects of bladder medications include dry mouth, dry eyes, and constipation. Extended-release forms and topical options may cause fewer side effects. Drinking small amounts of water, chewing sugar-free gum, or using eyedrops can help relieve dryness.
Bladder injections
Botox (onabotulinumtoxinA) injections into the bladder muscle can relax it and increase its capacity. The effects may last six months or longer, after which another treatment is needed. Some patients may experience urinary retention or urinary tract infections after injections.
Nerve stimulation
Electrical stimulation can help regulate nerve signals that control bladder function.
-
Sacral nerve stimulation: A thin wire is placed near the sacral nerves in the lower back. If the test procedure improves symptoms, a small device is implanted to deliver continuous electrical pulses.
-
Percutaneous tibial nerve stimulation (PTNS): A thin needle near the ankle delivers gentle electrical impulses to the tibial nerve, which communicates with bladder control nerves. Weekly sessions are done for 12 weeks, followed by maintenance treatments every few weeks.
Surgery
Surgical options are reserved for severe cases that do not respond to other treatments. Procedures include:
-
Increasing bladder capacity using sections of the bowel.
-
Removing the bladder and reconstructing a new one (neobladder) or creating an opening (stoma) to attach a urine collection bag.
These surgeries are major procedures and are considered only when all other treatments fail to provide relief.
Advertisement